Students Experience Cardiovascular Care Firsthand
 For IU Health Methodist, which treats the highest volume of patients on cardiac support devices in Indiana, the collaboration with the Weldon School is integral to their plans for developing a world-class cardiovascular program.
For IU Health Methodist, which treats the highest volume of patients on cardiac support devices in Indiana, the collaboration with the Weldon School is integral to their plans for developing a world-class cardiovascular program.
Mike Wagoner, executive director of the IU Health cardiovascular strategic service line, explains that modern cardiovascular care requires that hospitals deploy new technology rapidly, and engineers need to see how that happens in the real world of clinical practice. The Weldon partnership provides a perfect mechanism for training engineers in the clinical setting.
“It’s time for engineers to move out of basement equipment repair shops and into the realm of bedside care,” Wagoner says.
Craig Goergen, assistant professor of biomedical engineering at Purdue, has been instrumental in developing the program, now in its third year. “It’s a competitive internship because many of our students are eager to learn how engineering can influence patient care,” he says.
“We don’t necessarily select students with the highest GPA,” Goergen continues. “Instead, we look for students who are really interested in medicine and in understanding how cardiovascular health can be improved by biomedical devices.”
Spring semester exposure
The internship program begins in May, with an intensive two-week course at IU Methodist Hospital. During this “Maymester exposure event,” up to six biomedical engineering students attend clinics, watch surgeries, visit the intensive care unit, and meet with patients and their families to learn about all aspects of cardiovascular medical practice. Students observe dozens of treatments and presentations by physicians and technicians.
 Summer internship
Summer internship
Next, one of these students is selected for a paid summer internship at Methodist Hospital — a rare and valuable experience for an undergraduate. The intern gets to observe clinicians in their daily routines: completing patient rounds, carrying out interventional procedures with varying degrees of invasiveness, and performing open-heart surgery. Students watch device implantation and heart-transplant operations.
“It’s like a real job,” says registered nurse Michelle Hare, director of Cardiovascular Statewide Strategy at IU Health Methodist and director of the internship program at Methodist. “They get exposure to real problems.” In one instance, the engineering students noticed a difficulty with a cardiopulmonary bypass system: blood was clotting in the extracorporeal tubing. Solving that problem became their senior design project.
Purdue biomedical engineering student Mary Christy was selected as a summer intern in 2015. “Being able to see imaging modalities and assist-devices actually in practice took our learning to a new level,” she says. “It allowed us to gain a much deeper understanding of their mechanisms — including seeing potential areas for improvement in these devices, which, for engineers, was very exciting.”
Fall study
In the next phase, summer interns, typically in their senior year, transition into working part time at Methodist hospital during the fall semester, performing duties like hosting observational events and managing the distribution of supply donations.
Interns also assist faculty members with clinically relevant research, such as analyzing records to compare IU Health Methodist program outcomes between various treatment methods, or bringing engineering skills to ongoing studies with IU Health investigators.
Spring leadership
With a year’s worth of exposure to cardiovascular care and experience in research, the seasoned intern assists the faculty and staff of Purdue and Methodist in designing the curriculum for next year’s “Maymester” course — for preparing the next crop of biomedical engineering interns.
“Our interns set the standard for excellence,” Hare says.
Some Purdue interns, like Mary Christy, are interested in pursuing medical practice as a career. Others look forward to careers in biomedical device design.
Future learning and practice
For the Weldon School, the IU Health Methodist partnership offers an opportunity to train and produce biomedical engineers with real-world experience in cardiovascular device development and implementation.
For IU Health, the partnership provides a pool of valuable expertise with which to build a world-class cardiovascular program.
“We envision a cross-collaboration model between engineers and surgeons,” says I-wen Wang, cardiothoracic surgeon at IU Health Methodist Hospital. “We foresee a consultative model, where engineers and physicians can work together on devices.”
Global experience, global impact
For the state of Indiana, the partnership could have tremendous benefits. Medical device companies and research institutes in China, for example, already have expressed interest in partnering with IU Health and the Weldon School with hopes of creating a global partnership capable of improving cardiovascular clinical care for patients worldwide.
Top photo: Mary Christy, now completing her senior year in the Weldon School, gears up for the operating room where she’ll observe an open-chest heart procedure.
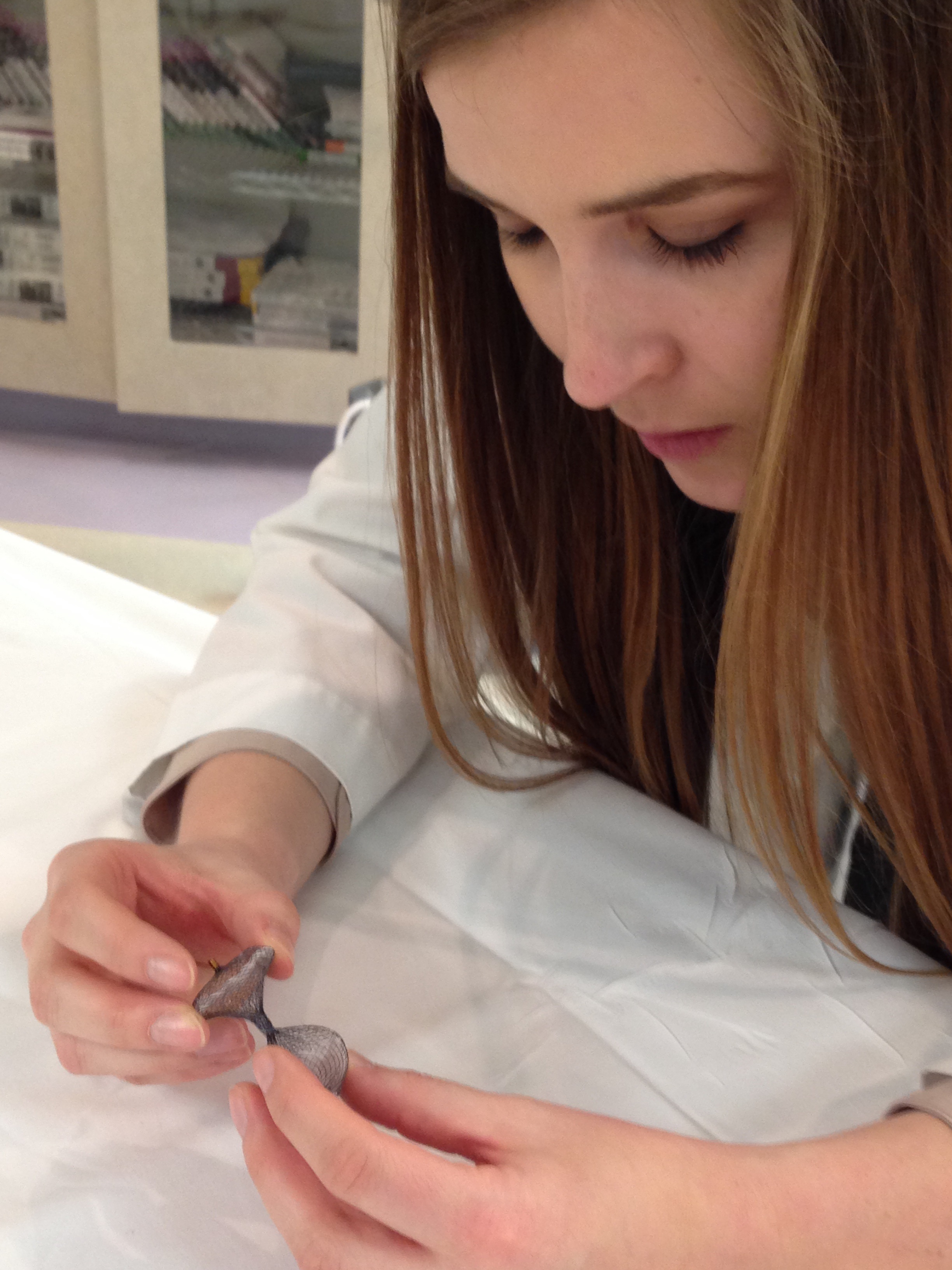
Bottom photo: Mary Christy examines a septal occluder, a device used to close an abnormal opening in the wall between the left and right side of the heart.